AI Isn’t Skipping Rural Healthcare—But It Is Arriving Differently
By First Products on Feb 10th 2026
There is a lot of buzz in the news about what infrastructure is needed to sustain AI at the scale it is growing. Healthcare entities, whether urban or rural, must address the costs of new AI-enabled technologies and the broadband and other considerations necessary for the tools to run at peak performance when deployed. Critical to universal adoption is the ability to bring the innovation to rural and underserved areas. Academic Medical Centers (AMCs) play a significant role in making this happen.
AMCs have become the proving ground for many AI tools. Tools developed for these centers are validated through use and later deployed to other parts of the network. What AMCs build or refine eventually become the very tools, like commercial software modules, cleared by the FDA. These modules with AI capabilities are being embedded into regulated medical devices sold by major vendors to rural healthcare systems, often bundled into equipment purchases. This innovation process brings critical functionality, powered by AI, into rural hospitals without the need for heavy AI investment, such as in-house data science teams or pilot programs.
AI Hides Inside Everyday Tools
AI is increasingly embedded in clinical documentation tools, scheduling systems, capacity planning systems, and remote patient monitoring platforms. A rural clinic may say, “We don’t use AI,” while actively relying on AI-driven alerts or recommendations. Invariably, the rural hospitals are buying products they need, often as part of a broader system upgrade, creating an invisible AI infrastructure of sorts. These AI-enabled tools can include, among others:
- Imaging equipment (AI-assisted reads, triage flags)
- Remote patient monitoring devices
- Clinical documentation tools
- Smart scheduling and staffing tools
“Adopting AI” becomes simply buying newer versions of familiar tools with AI embedded.
What’s Driving AI Access in Rural & Underserved Care
Many rural and critical access hospitals are affiliated with larger systems, are a part of regional networks, or use shared EHRs and vendors. When AI is deployed at the system level, it flows outward. This reduces risk for rural entities, as the governance, training, and contracts are already in place through the affiliation.
The telehealth expansion has normalized adoption in many respects. This revolution has equipped rural communities with remote diagnostics, virtual consultations, and centralized expertise to support decentralized care. AI fits naturally into this model for applications like:
- Pre-analyzing data before a remote specialist sees it
- Flagging high-risk patients
- Supporting non-specialist clinicians with decision support
The technology brings efficiency, but that isn’t the whole picture. For instance, in areas where fewer specialists are available or nurse-to-patient ratios are higher, AI-enabled tools can serve as practical clinical support, helping small, overburdened staff do more.

A Quick Look at Rural Disparities
As expected, AI adoption lags substantially in rural and smaller facilities compared to larger or urban peers. The American Hospital Association (AHA) reports ~56 % usage of predictive AI compared with 81 % for urban hospitals. And in critical access hospitals, in tiny facilities serving remote areas, it is reported that adoption is ~50% versus ~80% at non-CAH hospitals.
One AHA survey of nearly 1,000 rural health leaders found that only about 8% of rural or critical access hospitals were using AI-driven analytics tools, a percentage far below broader hospital benchmarks. Healthcare Brew
Friction Still Exists (and It’s Not Just Budget)
Access to AI is still gated by access to infrastructure, which is troublesome for rural communities that may face inconsistent broadband, aging hardware, or limited IT support staff. Additionally, learning to trust the results is a significant factor, as it is with AI across all markets. Rural clinicians may want to understand why a recommendation is made, or how to validate output and assumptions, since liability feels more personal when teams and resources are limited.
Another consideration is the rural hospital's ability to manage change. Even a good AI use case can fail without critical onboarding policies, clear workflows, or minimal training overhead, limiting rural communities to perhaps simpler solutions. And if the AI tools are built on populations or datasets that differ from those in rural settings, the results may look very different from their worldview, diminishing provider trust in the tools. For any AI-enabled tool to succeed, it will always need to support, not replace, caregiver and technician expertise and judgment.

Summing It All Up: Where AI Is Heading for Rural Healthcare?
The pundits are all discussing the massive infrastructure needs of large-scale AI. But for the rural healthcare providers, AI is already here. This can lessen the pressure of handling what is perceived as a quite complex shift in critical care delivery. AI will continue to be deployed in devices in rural areas, not as standalone systems. Equally, the vendors understand that the system needs to operate faultlessly across diverse end locations and can design for low-bandwidth, for example. Federal broadband and telehealth investments could also strengthen digital infrastructure in underserved regions.
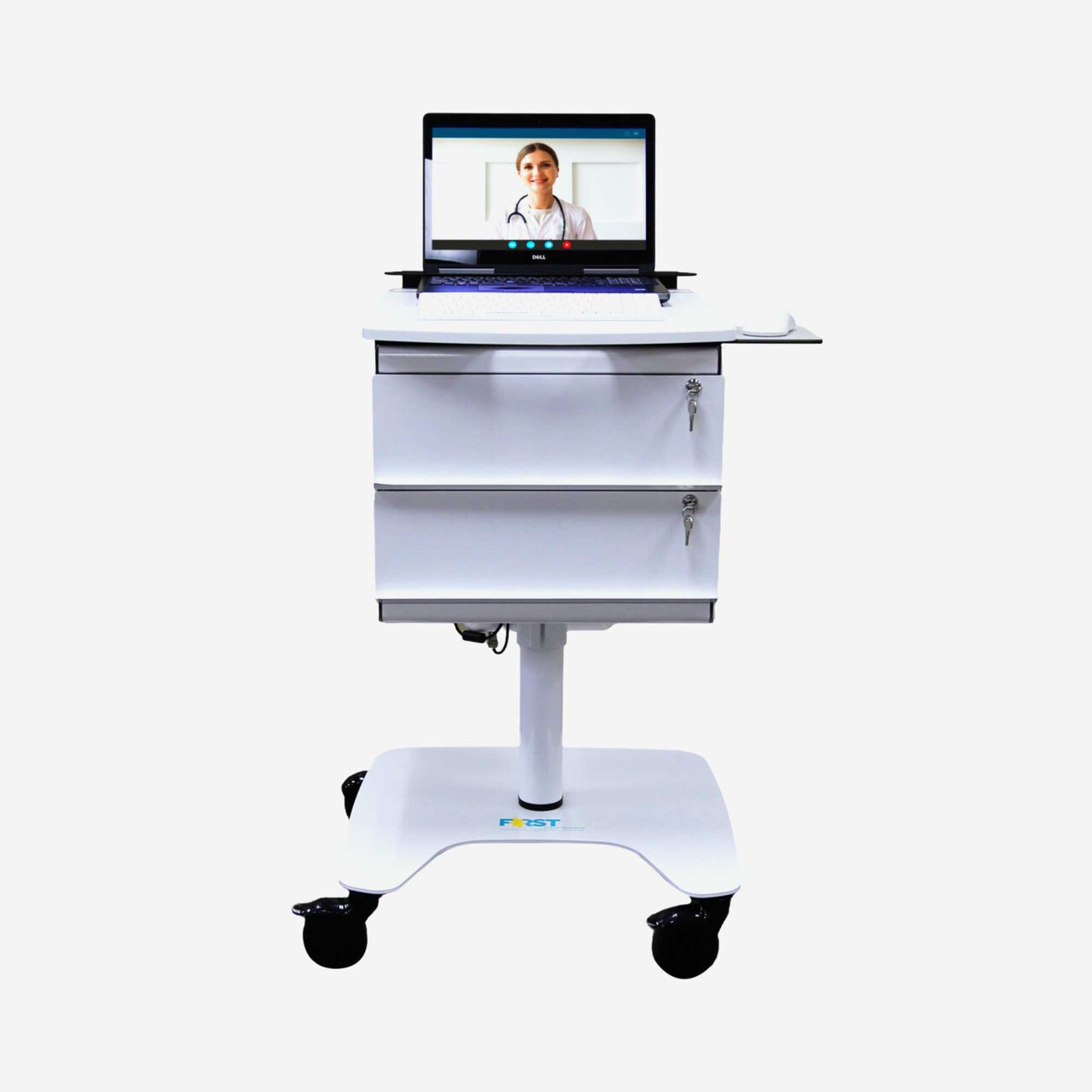
Making AI accessible to underserved communities is about designing it to meet care teams where they already are. Integrators creating bundled solutions know this. By working with manufacturing partners, they can deliver complex solutions via medical equipment, such as mobile carts, that caregivers already use in workflows, minimizing interruptions to existing protocols to accommodate new tech-enabled tools.
Be assured, First continues to work with enterprise-level hospitals, AMCs, and solution Integrators to create custom mobile carts, maintaining a strong commitment to high-quality product manufacturing and delivery to any community being served.
We’re showcasing our CODESIGNLIVE Sessions at VIVE and HIMSS. These unique 15-minute meetings illustrate the real power of collaborative, custom design, taking your technology-enabled mobile cart solution from vision to a caregiver powerhouse.